Signs Of Weak Pelvic Floor After Childbirth And Recovery
After childbirth, many women notice changes they weren’t prepared for. Urine leaks when you laugh, pressure in your pelvis, or a heavy, uncomfortable sensation can show up weeks or even months later.
These signs of weak pelvic floor after childbirth are easy to dismiss, especially when you’re told they’re just part of recovery.
When these symptoms don’t fade, they begin to affect daily life. Exercise feels risky. Intimacy can become uncomfortable. Confidence drops, and many women stay silent, unsure if anything can truly help.
As physical therapists, we work with patients experiencing pelvic floor symptoms across many stages of life, including after childbirth. This article explains common pelvic floor symptoms after pregnancy, why they happen, and what recovery looks like.
What Happens to the Pelvic Floor After Childbirth
Pelvic floor post-pregnancy dysfunction refers to changes in strength, coordination, or support of the pelvic floor muscles after pregnancy and delivery.
According to clinical research, childbirth can lead to weakness, stretching, or injury of pelvic floor muscles and connective tissues, contributing to dysfunction in the postpartum period.
During pregnancy, the pelvic floor supports increasing weight as the uterus grows. Hormonal changes also affect connective tissue, allowing muscles and ligaments to stretch more than usual in preparation for delivery. This combination places prolonged load on the pelvic floor even before labor begins.
During vaginal delivery, the pelvic floor muscles lengthen significantly to allow the baby to pass through the birth canal. This stretching can temporarily reduce muscle strength, alter coordination, or irritate nearby nerves. In some cases, small muscle or connective tissue injuries occur, even without obvious tearing.
Everyday Signs of a Weak Pelvic Floor After Birth
A weak pelvic floor can affect support and control during everyday activities. These signs often appear during movement, pressure, or fatigue and may become more noticeable as the day goes on.
Common signs include:
Urinary leakage with activity: Urine leaks during coughing, sneezing, laughing, jumping, or running. This happens when weakened pelvic floor muscles cannot maintain closure as pressure increases.
Heaviness or pressure in the pelvis: A dragging, full, or “bulging” sensation may be felt in the vagina, often worsening by the end of the day. This can be related to reduced support of the pelvic organs.
Difficulty fully emptying the bladder: Some women feel persistent urgency after urinating or the need to strain. Changes in pelvic support can affect how the bladder empties.
Pain or discomfort with intercourse: Reduced muscle support or coordination may contribute to discomfort, decreased sensation, or difficulty during penetration.
Bowel control changes: Difficulty controlling gas or stool can occur when pelvic floor muscles and anal sphincters are not functioning optimally.
Hidden Signs of a Weak Pelvic Floor After Birth
Some pelvic floor symptoms are less obvious and don’t always point directly to pelvic health. Because they don’t fit common postpartum checklists, they’re often mistaken for unrelated issues or overlooked entirely.
Less visible signs can include:
1. Tampons Slipping Out or Not Staying in Place
Difficulty keeping a tampon in position can occur when pelvic floor support and vaginal wall tension are reduced. The pelvic floor plays a role in maintaining internal closure, and changes after childbirth can affect how well objects are held in place.
2. Vaginal Air Release (“Queefing”)
Uncontrolled release of air during movement, exercise, or intimacy can happen when the pelvic floor does not close effectively. While harmless, this may reflect reduced muscular control rather than a gynecological issue.
3. Urinary Urgency or Burning Without Infection
Symptoms that feel like a urinary tract infection but return with negative test results can be linked to pelvic floor dysfunction. Changes in muscle support or coordination can irritate surrounding tissues and alter bladder signaling.
4. Ongoing Hip or Tailbone Pain
The pelvic floor works closely with deep hip and pelvic muscles. When pelvic support is reduced, strain can shift to the hips, tailbone, or lower back, leading to pain that does not respond to typical orthopedic treatment alone.
5. Twitching or Fluttering Sensations in the Pelvic Area
Intermittent twitching or vibrating sensations can occur due to muscle fatigue or nerve irritation after childbirth. These sensations often increase with prolonged standing, physical activity, or overall fatigue.
Because these signs don’t always seem pelvic-related, they’re often attributed to aging, posture, or general postpartum recovery.
What Causes Pelvic Floor Weakness After Childbirth
Pelvic floor weakness after childbirth usually develops from a combination of pregnancy-related strain and delivery-related stress. Several factors can affect how well the pelvic floor recovers.
Common causes include:
Hormonal changes during pregnancy: Hormones such as relaxin increase tissue flexibility to prepare for birth, which can reduce pelvic floor support and muscle tension.
Prolonged load from pregnancy: As the baby grows, increasing weight places continuous strain on the pelvic floor muscles and connective tissues.
Vaginal delivery-related stretching: During birth, pelvic floor muscles lengthen significantly to allow delivery, which can temporarily reduce strength, coordination, or endurance.
Instrument-assisted delivery: Forceps or vacuum-assisted births place additional stress on pelvic floor muscles and nerves, increasing the likelihood of early weakness.
Multiple pregnancies or vaginal births: Repeated stretching over time can affect the pelvic floor’s ability to fully recover between deliveries.
Chronic straining or pressure: Constipation, frequent coughing, or sustained increases in abdominal pressure can further weaken pelvic support after childbirth.
Return to high-impact activity too quickly: Running, jumping, or heavy lifting before adequate recovery can expose weakness that was not obvious earlier
Who Is at Risk After Childbirth
Pelvic floor changes after childbirth are common, but some women are more likely to experience ongoing symptoms.
Research shows that up to 50% of women report pelvic floor dysfunction within 10 years of giving birth, highlighting how frequently these issues persist beyond early recovery.
Risk is higher with:
Instrument-assisted delivery (forceps or vacuum)
Multiple vaginal births
Higher body weight
Chronic constipation or frequent straining
Chronic coughing
Symptoms don’t always appear right away. Many women feel fine at their six-week postpartum visit, then notice changes later when returning to exercise or higher-impact activity.
Despite how common this is, most postpartum women do not receive pelvic floor physical therapy, often because symptoms are dismissed as normal or care is delayed. Earlier evaluation can help guide recovery and reduce long-term impact.
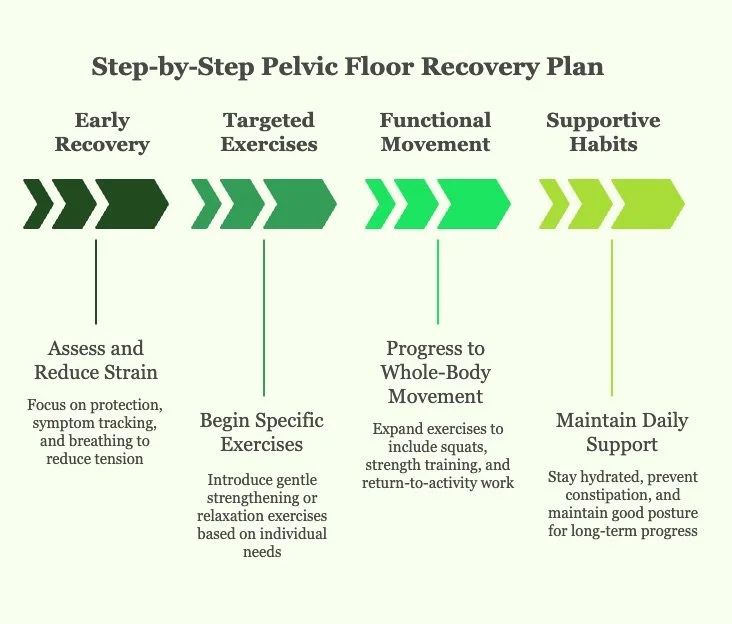
Your Step-by-Step Recovery Plan
Pelvic floor recovery works best when it’s gradual and guided. The goal is to restore coordination, strength, or relaxation based on how your pelvic floor is functioning.
Step 1: Assess and Reduce Strain
Early on, the focus is protection and awareness. This may include tracking symptoms, limiting high-impact activity, and using breathing techniques to reduce unnecessary tension and pressure.
Step 2: Begin Targeted Exercises
Once patterns are identified, exercises are introduced based on your needs.
A weak pelvic floor is addressed with gentle strengthening and coordination work.
A tight pelvic floor focuses on relaxation, breathing, and improving muscle length.
Step 3: Progress to Functional Movement
As control improves, exercises expand to include whole-body movement. Strength training, squatting, and return-to-activity work help the pelvic floor function during daily tasks and exercise.
Supportive Habits That Matter
Recovery is also influenced by daily habits. Staying hydrated, preventing constipation, and maintaining good posture can reduce unnecessary strain on the pelvic floor and support long-term progress.
Pelvic floor recovery takes time, but improvement is possible at any stage. A consultation with a physical therapist can help clarify what your pelvic floor needs and guide recovery safely and effectively.
When Postpartum Changes Need More Support
The signs of weak pelvic floor after childbirth can show up in everyday activities and affect comfort, movement, and confidence. These changes are common after pregnancy and delivery, but they aren’t something you have to accept or ignore.
Understanding what’s happening in your body is the first step toward meaningful improvement. Recovery works best when it’s guided and specific to your needs. A physical therapist can assess pelvic floor function and help you move forward safely.
If pelvic floor symptoms are affecting your daily life, reach out today to start the next step in recovery.
Frequently Asked Questions
Can a weak pelvic floor cause lower back pain after childbirth?
Yes, weak pelvic floor strains core and back muscles like multifidus, causing overcompensation and chronic pain. Integrated exercises and PT restore balance in 8-12 weeks for lasting relief.
How do I tell if my pelvic floor is weak or tight postpartum?
Pain with sex, tampons, or urgency signals tight, while painless leaks or heaviness mean weak. PT internal exam confirms accurately, seek early for tailored treatment and faster recovery.
Is it too late to fix my pelvic floor years after giving birth?
No, muscles retrain effectively anytime, even post-menopause, with consistent therapy. 80% of women improve significantly decades later, start now to regain confidence in activity and intimacy.
Why do my tampons keep falling out after childbirth?
Weak vaginal walls from laxity or mild prolapse can't grip securely, classic hypotonic sign. Targeted strengthening via PT restores tone in months; early action prevents worsening.
Will signs of weak pelvic floor resolve on their own after pregnancy?
Rarely. 50% persist 10 years without intervention as pregnancy trauma lingers. Proactive PT halves risks and speeds full recovery; don't wait, act today for best results.